ICD-10 Codes: Include the medical code for MSA (G23.8)
Multiple System Atrophy (MSA)

What is (MSA)
Multiple System Atrophy?
Multiple System Atrophy (MSA) is a rare, progressive, and terminal neurological disease that affects multiple systems of the body—most notably movement, balance, blood pressure, and autonomic functions such as breathing, bladder control, and heart rate.
MSA is classified as an Atypical Parkinsonian Disorder, meaning it shares symptoms with Parkinson’s disease but progresses differently, responds poorly to Parkinson’s medications, and involves more widespread neurological damage.
There is currently no cure, and treatment focuses on managing symptoms and preserving quality of life.
March is Multiple System Atrophy (MSA) Awareness Month. A month dedicated to shining light on a rare, aggressive, and often misunderstood neurological disease that affects thousands of families worldwide — including mine.
Why MSA Used to Be Called:
Shy–Drager
syndrome.
Before being fully understood, MSA was often referred to as Shy–Drager Syndrome, named after:
In 1960, these physicians first described patients who had:
-
Severe autonomic nervous system failure
-
Blood pressure drops upon standing (orthostatic hypotension)
-
Parkinson-like movement symptoms
As research advanced, doctors realized Shy–Drager Syndrome, striatonigral degeneration, and olivopontocerebellar atrophy were all part of the same disease spectrum, now unified under the name Multiple System Atrophy.
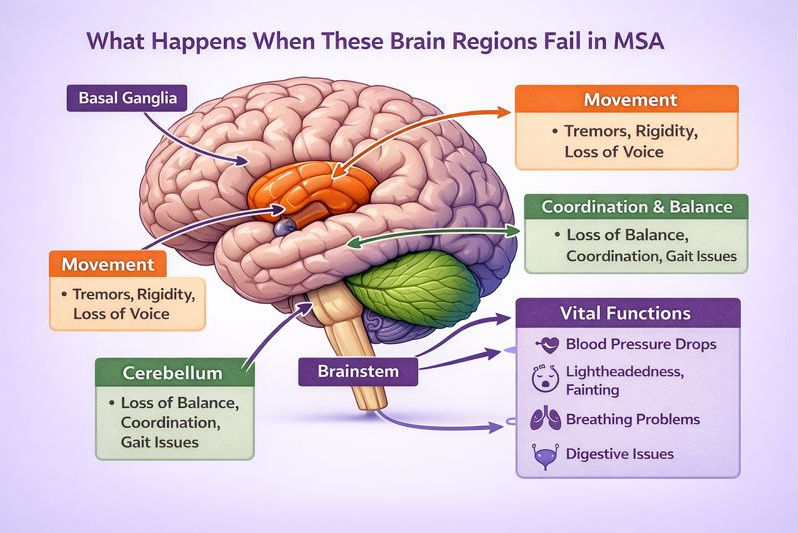
What Happens as MSA Progresses
MSA affects the autonomic nervous system, which controls functions most people never think about. As those systems begin to fail, symptoms may include:
Blood Pressure & Heart Regulation
-
Sudden drops in blood pressure when standing
-
Dizziness or fainting
-
Extreme fatigue
-
Blackouts
Balance & Movement
-
Loss of balance and coordination
-
Frequent falls
-
Muscle rigidity and stiffness
-
Difficulty walking
-
Wheelchair dependence
Speech & Swallowing
-
Slurred or slowed speech
-
Weak voice
-
Choking or aspiration
-
Difficulty swallowing (dysphagia)
Breathing & Sleep
-
Sleep apnea
-
Stridor (high-pitched breathing sounds)
-
Shallow or irregular breathing
-
Increased risk during sleep
Cognitive & Emotional Impact
-
Anxiety and depression
-
Emotional flattening
-
Frustration due to loss of independence
-
Grief over loss of identity and abilities
Bladder, Bowel & Sexual Function
-
Loss of bladder control or urinary retention
-
Constipation
-
Sexual dysfunction
-
Loss of temperature regulation
Importantly, intelligence is often preserved, meaning individuals with MSA are fully aware of what is happening to their bodies.
Living With MSA
MSA doesn’t just affect the person diagnosed—it impacts:
-
Spouses
-
Children
-
Caregivers
-
Families
-
Entire support systems
Living with MSA requires:
-
Adaptive equipment
-
Multidisciplinary medical care
-
Emotional and mental health support
-
Advocacy and awareness
Why Awareness Matters
Because MSA is rare, many doctors may never see a case in their careers. Awareness leads to:
-
Earlier diagnosis
-
Better symptom management
-
Increased research funding
-
Improved support for patients and families